ПЕДИАТРИЯ
Rikhsiev U.Sh., Mannanov A.M., Rakhmankulova S.A.
Desquamative erythroderma of Leiner-Mussu,
a rare and severe disease of newborns. The description
of clinical case, course, complex of therapeutic and
prophylactic measures in dexvamatic erythroderma
Leiner-Mussu is presented. This is a rare severe disease
of children of the first 3 months of life, which in case of
untimely diagnosis and inadequate treatment can be
fatal, and therefore it is important to timely recognize
the dermatosis and refer sick children for treatment in
hospital, which will significantly increase the chances
of recovery. The unclear etiology, pathogenesis and
rarity of occurrence presents difficulties in diagnosis
and treatment. Erythroderma Leiner-Mussouw,
diagnosis, clinic and treatment.
Erythrodermia
desquamotiva
Leiner-
Mousslous -
was first isolated as a separate nosological
unit by French pediatrician Mousslous in 1905 and
described by Austrian pediatrician Leiner in 1907.
Leiner-Mousslous
dexvammatory
erythroderma (DELM) is a rare severe disease of
children in the first 3 months of life. The etiology of the
pathogenesis of DELM is not completely clear. The
disease is considered as a generalized form of
seborrheic dermatitis, its erythrodermic variety. The
prevailing opinion is that seborrheic dermatitis under
unfavorable conditions can transform into DELM
[1,2,4,5]. One of the main causes of DELM
development is considered to be auto-intoxication,
because skin lesions are aggravated with the severity of
gastrointestinal tract disorders [3], associated with a
decrease in the enzymatic activity of the intestine and
wall digestion leading to a violation of protein and lipid
metabolism. It should be noted that in the causes of
DELM besides intoxication with products of disturbed
metabolism, an important role is played by feeding with
qualitatively inferior mother's milk, with a reduced
content of biotin, vitamins of the B group (B2, B6, B12),
A, E, C [1,5,6]. It should be noted that the disease is
more characteristic of breastfed children, more often
girls. The disease is aggravated by pyococcal and
candida infection, which have a sensitizing effect on the
div [6,7]. Some researchers consider DELM an
independent disease [6].
The main skin signs of DELM are flaky
erythroderma, and diarrhea and nutritional disorders
(hypotrophy) in the GI tract. The disease more often
begins in the 3-4th week of life with dyspeptic disorders
(frequent regurgitation, vomiting, frequent liquid
stools). The skin process more often begins in the
buttocks, groin and hip folds with the appearance of
bright red flaky foci, and sometimes the pathological
process can begin with the scalp, moving to the neck,
upper torso, axillae, descending into the anogenital area.
Within a few days, most of the skin becomes brightly
hyperemic, covered with papillary and lamellar
abundantly flaky che-shuiki, except for small islets of
unaffected skin. In the area of cervical, axillary and
inguinal-femoral folds there are skin maceration with
formation of cracks and wetting. The scalp is covered
with multilayered thick scales - crusts, grayish-yellow
and brownish color in the form of a shell, descending on
the forehead, supraorbital arches with spreading to the
occiput. Temporary baldness is possible. Scales can be
removed, but soon they reappear. The skin under the
scales is hyperemic with infiltration. Pathologic
changes in the skin may persist for an average of 1
month. Mucous membranes, hair and nails are not
affected.
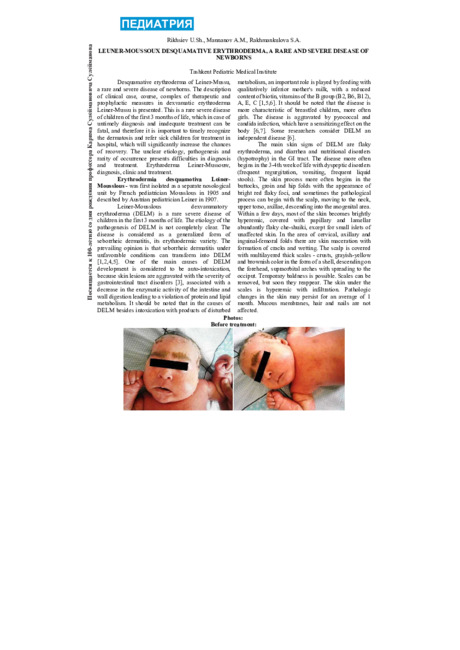
Photos:
Before treatment:
П
ос
вя
щ
ае
тс
я
к
1
00
-л
ет
и
ю
с
о
дн
я
ро
ж
де
н
и
я
п
ро
ф
ес
со
р
а
К
ар
и
м
а
С
ул
ей
м
ан
ов
и
ч
а
С
ул
ей
м
ан
ов
а
LEUNER-MOUSSOUX DESQUAMATIVE ERYTHRODERMA, A RARE AND SEVERE DISEASE OF
NEWBORNS
Tashkent Pediatric Medical Institute

Посвящается к 100-летию со дня рождения профессора Карима Сулеймановича Сулейманова
31
5

ПЕДИАТРИЯ
Timely adequate treatment in the hospital
provides cure within 2-4 weeks. The complex of
treatment and rehabilitation measures includes
normalization of feeding of the child (caloric
vitaminized food of a nursing mother, additionally
vitamins C, B, A), broad-spectrum antibiotics
(lincomycin, gen-tamycin, ampicillin, cephalosporins),
glucocorticosteroids,
desensitizing
drugs,
hemotransfusions, immunocorrective drugs, pro and
prebiotics, enzymes that help and improve digestion.
Properly conducted topical therapy is of great and key
importance, it should include combined ointments and
creams with anti-inflammatory, antibacterial, antifungal
and epithelializing action.
Here is our observation:
Patient A. I/B
#230/82 was born on 06.06.23. From Kashkadarya
region, admitted to the infant department of pregnancy
of 2 births, pregnancy was toxicosis, the of 3,500 grams.
The child grew and developed normally until 25 days of
age, breastfed, skin was clear. At the age of 25 days, the
child had green, frequent, liquid stools and at the same
time in the area of large folds appeared pronounced
redness with wetting. We applied to the pediatrician in
the SVP at the place of residence, who recommended
topical ointment sinoflan, for 3-4 days erythema seized
almost the entire skin, after which the child was referred
to a dermatologist in the district clinic, where the child
was
diagnosed:
Congenital
ichthyosis
with
hospitalization in the hospital, but the child's condition
did not improve and the parents arbitrarily took the child
home and turned to the local "tabib", which as a
treatment recommended to smear the whole div with
plain sour cream with the addition of red ground pepper,
which the parents did. The next day the child developed
high fever, adynamia, erythematous areas covering the
whole div became wet and covered with layered
crusts. Due to the severity of his condition, the child was
hospitalized in the children's somatic department of
Chirchik city
.
Where, according to the mother, the child
received benzylpenicillin every 6 hours for several days
and topical ointment Dermoveit. Again, the parents took
the child away from the medical institution of their own
volition due to further deterioration of the child's
condition without discharge and applied to the clinic of
TashPMI, where the child was hospitalized in the infant
department in an emergency order on 22.09.23.
П
ос
вя
щ
ае
тс
я
к
1
00
-
Tashkadarya PMI on 22.09.23. child from the 2nd
child was born on time, physiologically with weight

At the time of admission, the general condition of the
child due to general intoxication is extremely severe,
passive and tearful, there was an affection of almost the
entire skin in the form of continuous erythroderma
covered with large scales. In the area of cervical,
axillary and inguinal folds there were wet erosions and
linear fissures, the scalp and supraorbital arches were
covered with multilayered serous-purulent crusts in the
form of a "helmet". Breathing through the nose was
difficult, rapid with signs of dyspnea and pronounced
perioral cyanosis. auscultation in the lungs hard
breathing. After a review radiograph of the lungs,
ultrasound, laboratory tests, examination of allied
specialists: pediatrician, surgeon and dermatologist, the
diagnosis was made: Desquamative erythroderma
Leiner-Mussu, complicated by pyoderma with
concomitant acute bilateral focal bronchopneumonia.
General therapy: cefatoxime 200mg per 50.0ml
of saline solution x 2p.v.d v/v; 30% sodium thiosulfate
solution 1.0 ml per 30.0ml of saline solution v/v;
dexamethasone 4% 0.3 ml v/v; Drotaverine 2% 0.2 +
dimedrol 1% - 0.2 per 2.0ml of saline solution v/v;
albumin 10% of saline solution v/v #1; plasma
transfusion #1 Per.os: fenistil 0% 0.2 + dimedrol 1% -
0.2 per 2.0ml of saline solution v/v. v/v; albumin 10%
solution v/v №1; plasma transfusion №1 Per.os:
phenistil 0.1% 2 drops x 2p.v.d.; bifobalance - baby 1
sachet x 2 p.v.d.; Creon 1/3 cap. x 3p.v.d.; asparkam %
tablet x 1p.v.d.; aevit 1 drop x 1p.v.d. Inhalations and
sanitation of the upper respiratory tract.
Topical combined therapy: methylene blue 1% (for
cracks and wetting), "candida" powder (in the area of
large folds), ointment "levamikol" + l-t "Vishnevsky"
(1:1) for crusts under / bandage, cream "triderm" + zinc
ointment (1:1) for redness and erosions. On the 7th day
from the beginning of intensive therapy the general
condition of the child began to stabilize, signs of
dyspnea disappeared, redness and swelling of the skin
decreased. On the 11th day the general condition
became satisfactory, the scalp and supraorbital arches
were significantly cleared of crusts. On the 17th day
hyperemia in the lesions was gone, erosions and fissures
were covered with epithelium, the child gained weight
and was discharged home in satisfactory condition. It
was recommended to continue supportive therapy and
follow-up with the pediatrician and dermatologist at the
place of residence.
The present publication and the described clinical
observation will be useful for physicians, it will help
them to be prepared to meet this rare, severe and
complex nosologic form for timely and adequate
treatment in order to achieve the fastest clinical effect
and to avoid many complications and unjustified
therapeutic measures. Prevention of DELM should start
from the antenatal period and include rational nutrition
of the pregnant and later lactating mother (complete,
balanced, rich in vitamins), adequate regimen and
proper care of the newborn.
Literature
1.
Zverikova F.A. Diseases of the skin of children. St. Petersburg: Sotis. 1994:172-175.
2.
Popkhristov P. Skin diseases in childhood. Sofia. 1963:236-238.
3.
Atlas Ya. Е. Skin diseases of the early infantile age. М 1961.
4.
Studenikin M. A. Handbook of pediatrician. M: Ellis lac. 1994;313- 314.
5.
Reference book. Edited by O.L. Ivanov. Skin and venereal diseases. Moscow: Medicine. 1997;331-332.
6.
Skripkin Y.K., Zverikova F.A., Sharapova G.Y., Studnitsin A.A. Manual of pediatric dermatology. Moscow:
Medicine. 1983;88-92.
7.
Mannanov A.M., Khaitov K.N. Bolalar teri va tanosil kasalliklari. Toshkent. 2016:560.
8.
Ashurova, D. T., and D. I. Ahmedova. "Hormonal adaptation features and neonatal period of newborn children
depending on the div weight at birth." World Healthcare Providers Multidisciplinary medical journal USE (2012):
41-44.
9.
Акрамова, Х. А., and Д. И. Ахмедова. "Характерные особенности плацентарного фактора роста при
задержке внутриутробного развития плода." Педиатрия 3-4 (2014): 29-31.
10.
Ahmedova, D. I., and Rahimjanov Sh A. Growth. "development of children. Methodical recommendation."
(2006): 3-82.
11.
Хакимова, Г. Г., А. А. Трякин, and Г. А. Хакимов. "Применение ниволумаба при раке толстой кишки с
синдромом Линча. Клиническое наблюдение." Злокачественные опухоли 10.1 (2020): 41-48.
П
ос
вя
щ
ае
тс
я
к
1
00
-л
ет
и
ю
с
о
дн
я
р
ож
де
н
и
я
п
ро
ф
ес
со
р
а
К
ар
и
м
а
С
ул
ей
м
ан
ов
и
ч
а
С
ул
ей
м
ан
ов
а